Aboriginal health
To Aboriginal people, health is about getting a balance between physical, mental, emotional, cultural and spiritual health. But numerous challenges make this a difficult goal.
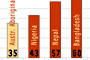
Selected statistics
- 2..3
- Aboriginal infant mortality rate compared to other Australians. 80% die under the age of one.
- 3
- Aboriginal death rate compared to the total Australian population.
-
44% - Percentage of adult (15-plus) Aboriginal people reporting 'excellent' or 'very good' health in 2008, unchanged from 2002. [1]
-
76% - Percentage of Indigenous infants (aged 0-3 years) who were breast-fed in 2008. [1]
- 36
- Times higher: The likelihood that sexually transmitted Gonorrhoea is prevalent in Aboriginal communities, compared to other communities. [2]
- 30
- Times higher: The likelihood that Aboriginal children suffer from anaemia and malnutrition due to iron deficiencies, compared to non-Aboriginal children. [3]
-
0.8% - Percentage of the overall Federal health expenditure in 2009 which was spent on Aboriginal health. [4]
- 7..12
- Times higher: The probability that 25-34 year-old Aboriginal Australians die from heart disease, compared to non-Aboriginal Australians. [5]
-
25% - Percentage of Aboriginal people who reported having used an illicit substance in the last 12 months (stable rate between 2002 and 2008). [6]
- 1.6
- Times higher: The probability that Aboriginal people have recently used cannabis, compared to non-Aboriginal people. [7]
- 1.95
- Rate at which Aboriginal people are hospitalised compared to non-Indigenous people.
- 125
- Number of Indigenous doctors practising in Australia, compared to 60,000 non-Aboriginal doctors. [8]
-
30% - Percentage of adults in Aboriginal communities suffering from type-2 diabetes. [9]
-
13% - Number of Indigenous homes having functioning water, waste, cooking and cleaning facilities (of 4,000 Indigenous homes surveyed during 1998-1999 in the Northern Territory).
- 6.5
- Times higher: The likelihood that an Aboriginal youth aged 15 to 24 as a sexually transmitted infection, compared to non-Aboriginal youth. [10]
-
60% - Percentage Aboriginal people are more likely to die from all cancer types than non-Indigenous people [11]. Cancer is the second leading cause of death for Aboriginal people.
- 6
- Times higher: The probability of sexually transmitted Chlamydia in Aboriginal communities, compared to other communities. [2]
-
83% - Percentage of Aboriginal children in the NT who had some decayed, missing or filled teeth. Average waiting time between referral and receipt of service: just over 14 months. [12]
-
46% - Percentage of Aboriginal people in 2018–19 who had at least one chronic condition that posed a significant health problem; rate in 2012–13: 40%. [13]
-
45% - Percentage of Aboriginal people aged 15 years and over who in 2018–19 rated their own health as excellent or very good; figure for 2012–13: 39%. [13]
- 2.3
- Times the 'burden of disease' is higher for Aboriginal people. [14]
List of articles
Aboriginal alcohol consumption

Aboriginal life expectancy

Aboriginal mothers and children

Aboriginal people with disability

Aboriginal sexual abuse

Aboriginal sexual health

Aboriginal smoking: a serious health problem

Challenge: Eat healthy food in communities

Diabetes at crisis levels in Australia

Ear health and hearing loss

How Aboriginal people use health services

Kidney disease among Aboriginal people

Making health services work for Aboriginal people

Mental health and Aboriginal people

Petrol sniffing

Successful Aboriginal health solutions

Trachoma & eye health

Traditional Aboriginal health care

To us, health is about so much more than simply not being sick. It's about getting a balance between physical, mental, emotional, cultural and spiritual health. Health and healing are interwoven, which means that one can't be separated from the other.
— Dr Tamara Mackean, Australian Indigenous Doctors' Association [8]
Australia is the only place on the planet where Indigenous health and well-being are going backwards.
— Sydney Morning Herald in 2009 [15]
Aboriginal people's burden of disease
Health experts express a group's health with the burden of disease which is the "impact of a health problem as measured by financial cost, mortality, morbidity, or other indicators. It is often quantified in terms of quality-adjusted life years or disability-adjusted life years." [16]
Aboriginal people's burden of disease is 2.3 times the rate of non-Aboriginal Australians. [14]
The disease group causing the most burden was mental disorders and substance abuse (19%), followed by injuries (including suicide) (15%), cardiovascular diseases (12%), cancer (9%), respiratory diseases (8%), musculoskeletal conditions (7%), infant and congenital diseases (6%) and endocrine conditions (4%). Other conditions accounted for 20% of the burden.
Coronary heart disease (CHD), suicide & self-inflicted injuries, anxiety disorders, alcohol use disorders and diabetes were the leading specific diseases, together contributing 24% of the total burden.
Heart diseases
Cardiovascular disease (CVD)
Cardiovascular disease, where blood vessels are narrowed or blocked, is among the leading causes of death for Aboriginal people.
Almost 12% of Aboriginal people have a long-term heart or related condition, and the number of deaths from CVD is more than 3 times that of non-Aboriginal Australians. [17] In 2018-19, around 15% of Aboriginal people reported having cardiovascular disease, and CVD accounts for 5.4% of all Aboriginal hospitalisations. [18] The disease contributes to about one third of the life-expectancy gap.
The higher prevalence is attributed to a range of risk factors such as smoking and poor nutrition, but also socio-social factors such as social isolation and depression.
Heart disease mostly affects relatively young Aboriginal people aged between 15 and 29. [19]
Rheumatic heart disease (RHD)
Rheumatic heart disease (formerly known as scarlet fever) can be life-threatening. It is caused by untreated and repeated exposure to streptococcus bacteria which eventually damages the heart valves. Suffers have to take penicillin and avoid any public places that could hold germs.
While it's virtually eradicated from non-Aboriginal communities, Arnhem Land in the Northern Territory has the highest rate in the world. For 2013-2017, in QLD, WA, SA and the NT combined, there were 1,043 new rheumatic heart disease diagnoses among Aboriginal people, a crude rate of 50 per 100,000. [18]
The Aboriginal RHD rate is about 122 times higher than the rate for non-Aboriginal people and kills two young Aboriginal people every week. The average life span of someone with RHD is only 40 years, which contributes to Aboriginal people's much lower life expectancy. [20]
Compounding the problem, young doctors sent to remote Aboriginal communities fail to recognise the disease or its precursor, rheumatic fever, because it is no longer taught. [20]
Coronary heart disease (CHD)
Also known as Ischemic heart disease (IHD), coronary heart disease means there is inadequate blood supply (circulation) to a local area due to blockage of blood vessels which supply that area (ischemia). The disease commonly manifests as heart problems caused by narrowed heart (coronary) arteries that supply blood to the heart muscle. It is the usual underlying cause of a heart attack.
In 2018, coronary heart disease was the leading specific cause of death of Aboriginal people living in NSW, QLD, WA, SA and the NT. [18] This is because the risk factors for CHD are common among Aboriginal people: smoking tobacco, high cholesterol, high blood pressure, diabetes, being inactive, being overweight, an unhealthy diet, depression and isolation. [21]
Dental health
Can you believe that in the mid-1960s Aboriginal children had far better oral health than non-Aboriginal children? Today the opposite it true: Aboriginal children now have more than double the rate of dental disease as other children. [22] In 2014-15, 34% of Aboriginal children aged 4–14 years had tooth or gum problems (a decrease from 39% in 2008). [18]
Rates of dental decay in remote Aboriginal communities are often worse than 70%. [23] A 5-year study of children under 10 found that 78% of Aboriginal children had dental disease, compared with only half of other kids. [24]
In some communities "almost all of those [surveyed] children believed that dental pain was just normal". [25]
Such poor health is caused by a lack of fluoride in water supplies and poor diet, according to Prof Kaye Roberts-Thompson, a spokesperson for the Australian Institute of Heath and Welfare. A study suggests that socio-economic disadvantage is also playing a role. [24]
"Historical factors such as forced familial separation, efforts of assimilation, on-going problems with alcohol, domestic abuse and land ownership issues... also play important roles," the study says.
Some children are not taught to brush, or don't own a toothbrush because poor families have other priorities for their limited budget. [25]
Of children aged 12, nearly half had a history of dental decay in the permanent teeth. [23] In 2012-2014, 36% of Aboriginal children aged 6–14 years had tooth decay in their permanent teeth. [18] The average number of decayed, missing and filled teeth was 1.1.
Many communities also have limited access to dental services and need to wait weeks, months, or even years for a new set of dentures through the public health system. Mobile dental services servicing remote communities are far more effective. One Aboriginal-run program, which employs junior clinicians using portable equipment, delivered 47% more treatments at 25% of the cost. [25]
Dental problems often lead to tooth loss, difficulties with eating, problems with speech (which affects your ability to work and learn) and infections that spread to other parts of the body. [24] They can also cause extreme pain that disrupts sleep, and damages mental health, concentration and self-esteem.
Drugs & dealers in Aboriginal communities
The use of methamphetamine, or ice, in some communities has reached "epidemic proportions" and is at a "crisis point", with children as young as 12 being exposed to the drug. [26]
People in Aboriginal communities inject predominantly amphetamine-based drugs, whereas heroin is more prevalent among non-Aboriginal drug users. [27]
Dealers have been targeting Aboriginal youths who have an income through jobs. They sell them large amounts of ice, knowing the youths will rack up large debts, which their families need to pay.
"Ice is a huge problem in our community," says Andrew Jackomos, Victoria's Commissioner for Aboriginal Children and Youth. [26]
If health services don't address the crisis, HIV and hepatitis C could rapidly escalate in communities. [27]
Injecting is a major problem in Aboriginal and Torres Strait Island communities.
— Dr James Ward, South Australian Health and Medical Research Institute [27]
Scabies 'normal' in communities
Scabies, a microscopic mite, is estimated to infest more than two-thirds of children in remote communities in their first year of life. [28] Up to 70% of all children are affected, and the infection can lead to sepsis, rheumatic fever, acute kidney disease and rheumatic heart disease. [22]
It causes an itch that can expose them to bacterial infection and ultimately to lethal rheumatic heart disease. About 18 people die of the disease each year in the Northern Territory.
Scabies and skin sores are to common that they are often considered normal [in communities]," says Prof Jonathan Carapetis, head of Menzies School of Health Research in Darwin. [28]
Worryingly, crusted scabies is of particular concern, an extremely contagious infection where people are infested with thousands of mites compared with a more usual infection where a person might about 10 mites. Left untreated, around half of people with crusted scabies die within five years. [22]
To break the cycle of infestation would require medical treatment as well as changing housing, hygiene and behaviour. Such changes have to come from communities themselves to be effective.
Cancer
In 2018-19, about 1% of Aboriginal people reported having cancer. The most common cancers diagnosed were lung cancer and breast (females) cancer. [18]High smoking rates among Aboriginal people contribute to this pathology.
For 2013-2017, the age-standardised mortality rate due to cancer of any type was 238 per 100,000, an increase of 5% compared to 2010-2014. [18]
Cancer is the second leading cause of death for Australian children aged one to 14 years. Interestingly, Aboriginal children are 36% less likely to be diagnosed with cancer than non-Aboriginal children. [29] Mortality rates are about the same.
Leukaemia and tumours of the central nervous system were the most common cancers among Aboriginal children.
Head and neck cancers in Aboriginal people are as prevalent as in non-Aboriginal people, but more than twice as likely to be diagnosed at a later stage than non-Aboriginal people. [30] Differences are less for other types of cancer.
One reason might be that many Aboriginal people are reluctant to visit their doctor or hospital, especially if it is not making them feel welcome.
Cancer Australia has developed a guide about lung cancer specifically for Aboriginal people.
Cancer is not a modern-day disease. Researches found cancer in human and humanoid remains as old as 120,000 and 1.7 million years old. [31]
Why are Aboriginal cancer rates 8% lower than those of other Australians (19%)?
Show
Because Aboriginal people die young from other causes. [32]
More resources
The HealthInfoNet website is an award-winning resource translating knowledge and academic literature for Aboriginal health workers in Australia.
The site was started in 1997. Visit www.healthinfonet.ecu.edu.au for more information.